Missing a tooth changes small moments first.
You notice it when you chew on one side. You notice it in photos. You may even catch yourself smiling with your lips closed at dinner, at work, or while meeting neighbors around Vienna and Northern Virginia. Many people live with that frustration for months or years because they assume they’ve waited too long, lost too much bone, or are “not a candidate” for implants.
That assumption is often wrong.
Dental implant candidacy is rarely a simple yes-or-no label. It’s usually a health question with clear checkpoints and, in many cases, a path forward. Some people are ready right away. Others need a little groundwork first, such as gum treatment or bone support, before an implant can be placed safely.
If you’ve been searching for who is a good candidate for dental implants or wondering whether your age, bone loss, or dental history rules you out, the best place to start is with a clear explanation in plain language. That’s what this guide is for.
Restoring Your Smile and Confidence in Vienna VA
A lot of patients start in the same place.
They’re not thinking about titanium posts or 3D scans. They’re thinking about real-life problems. Biting into a sandwich feels awkward. A removable denture shifts at the wrong moment. A gap in the smile makes every social event feel a little more stressful than it should.

Why missing teeth affect more than appearance
Losing a tooth can change more than the way your smile looks.
It can affect the way you chew, the way you speak, and the way the rest of your teeth fit together. For some people, it also brings a quiet kind of self-consciousness that builds over time. They stop laughing freely. They avoid certain foods. They put off treatment because they’re worried the process will be complicated or painful.
That hesitation is understandable. Dentistry can feel technical fast.
A more reassuring way to think about implants
Dental implants are often the most complete way to replace a missing tooth because they’re designed to support a replacement tooth from the root area up, not just cover the space. That matters for comfort, function, and long-term stability.
Many patients who assume implants are out of reach turn out to be closer to candidacy than they think.
The key point is simple. Being a good candidate doesn’t mean having a perfect mouth. It means having, or being able to build, the right foundation for lasting success.
That’s why the conversation matters so much. A careful evaluation can show whether you’re ready now or whether a preparatory step could make implants possible later. For many adults in Vienna, VA, that shift in perspective is a relief. You’re not being judged. You’re being assessed thoughtfully.
The goal is a healthy, confident smile
If you’ve been comparing dentures, bridges, cosmetic options, or other restorative dentistry treatments, implants often come up because they solve both a cosmetic and functional problem at once. They can help a smile look natural again, but they also help restore the ability to chew and speak more comfortably.
That's why people ask about dental implants near me. They don’t just want a tooth replaced. They want to feel normal again.
Understanding Dental Implants The Gold Standard for Tooth Replacement
A dental implant replaces a missing tooth in the same basic order nature built it. First, a small post is placed in the jawbone where the root used to be. After that area heals, a connector and a custom crown are attached so the tooth looks and functions like part of your smile again.
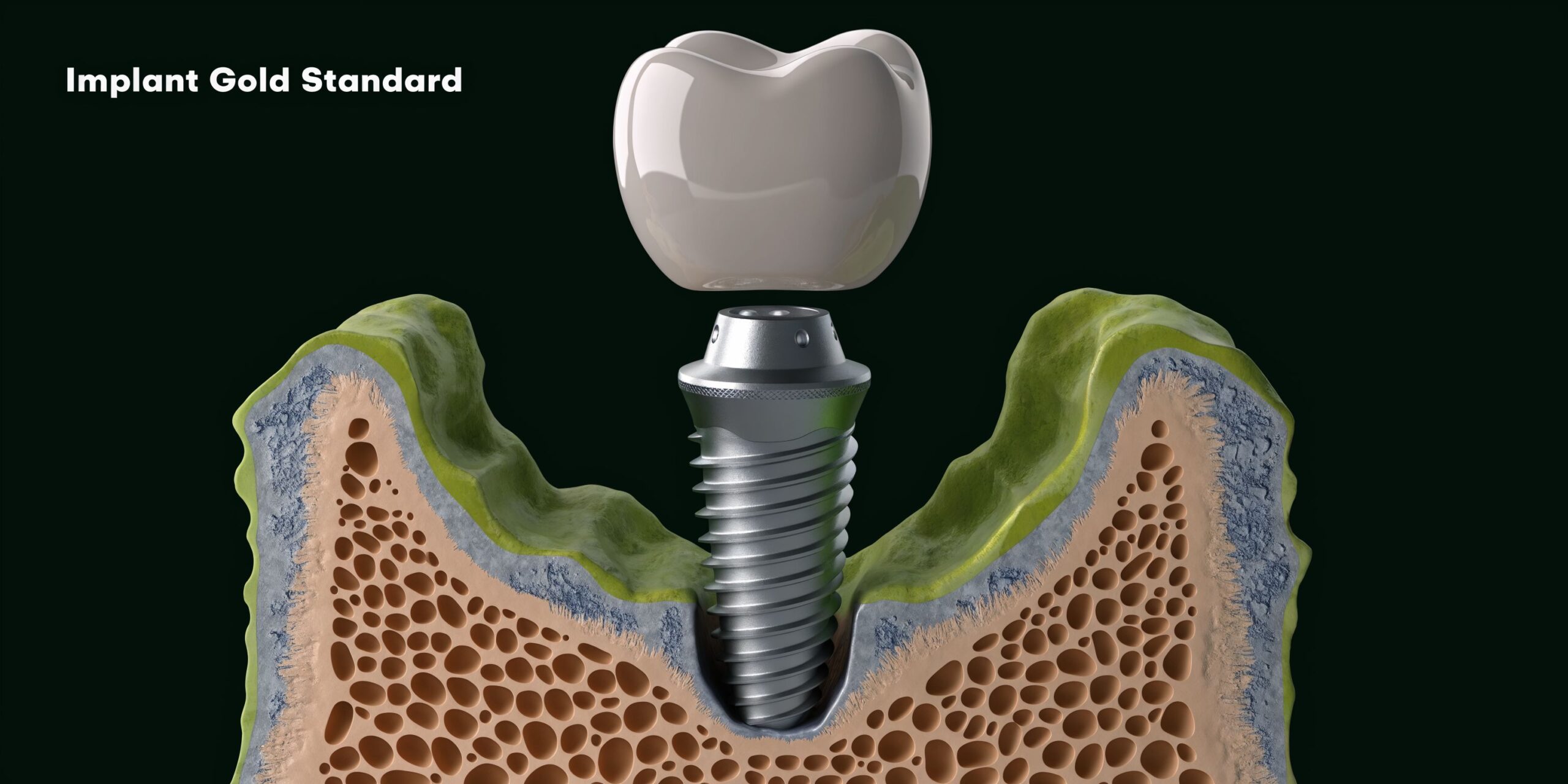
That root-first design is what makes implants different from other tooth replacement options. A bridge spans the space. A denture rests on the gums. An implant is placed in the jaw itself, which gives the final tooth a more grounded kind of support.
The three parts of an implant
Patients usually find implants easier to understand when the system is broken into three parts:
- The implant post sits in the jawbone and replaces the root.
- The abutment connects the post to the new tooth.
- The crown is the visible part above the gums, shaped and shaded to match nearby teeth.
An implant works like a house built on a foundation. The post is the base in the bone, and the crown is the part you see and use every day.
Why titanium is commonly used
The implant post is commonly made from titanium because the body generally accepts it well and because it holds up under chewing forces over time. The American Academy of Implant Dentistry explains that titanium has been widely used in implant dentistry for decades because of its strength and biocompatibility, as described in its overview of dental implant materials and treatment basics.
For patients, the message is simple. This is not an experimental material. It has a long clinical history.
What osseointegration means in plain English
Osseointegration is the healing step that lets an implant become stable.
After the post is placed, the surrounding bone gradually bonds to it. You can picture it like a fence post set into concrete. The post needs time to become firmly held in place before it can reliably support pressure from biting and chewing.
This is also why candidacy is often a journey, not a yes-or-no label on day one. If bone has shrunk after a tooth was lost, a patient may still become a strong implant candidate with preparatory care such as bone grafting to rebuild support for dental implants. In Vienna, VA, that is often the step that changes the conversation from "maybe not" to "very possible."
Why implants are considered the gold standard
Implants are often called the gold standard because they replace more than the visible part of a missing tooth. They restore support from the root area upward, which can improve stability, chewing comfort, and the way the tooth emerges through the gums.
That matters in daily life. Patients often want a replacement that feels secure when they eat, speaks clearly, and blends into the smile without drawing attention.
Implants also fit into larger treatment plans. One person may need a single implant and crown. Another may need gum treatment first, or grafting, or a combination of implants, crowns, and cosmetic work. General health also affects healing.
The most reassuring part for many patients is this. Implant candidacy can often be built. If the foundation is not ready today, treatment can often improve that foundation so implants become a realistic option later.
The Key Factors for Dental Implant Candidacy
Patients often ask the same direct question. Who is a good candidate for dental implants?
The honest answer is that dentists look at a few big categories, not one single detail. You don’t need a perfect dental history. You do need the conditions that help an implant heal and stay healthy.
Jawbone support matters
The first major checkpoint is bone.
A dental implant needs enough jawbone to hold it firmly during healing and long after treatment is complete. One technical benchmark for standard implants in the lower jaw is at least 10mm of height and 5mm of width, measured with 3D CBCT imaging, which also helps map bone density and important structures like nerves. That comes from clinical guidance on dental implant candidacy and CBCT planning.
That number can sound intimidating at first. It shouldn’t.
What matters most is not whether you can guess your bone level at home. It’s whether imaging shows enough support, or shows a way to create that support safely. Bone loss after a missing tooth is common because the jaw no longer gets the same stimulation in that area.
Gum health is part of implant health
Healthy gums matter because gums form the protective seal around an implant.
If there’s active gum disease, bacteria and inflammation can interfere with healing. That doesn’t always mean implants are off the table. It often means the gums need to be treated first so the mouth is healthier before surgery.
Patients sometimes focus only on the missing tooth. Dentists look at the whole environment around it.
- Stable gum tissue helps protect the implant.
- Low inflammation supports cleaner healing.
- Regular home care reduces the chance of future complications.
Your overall health influences healing
General health also plays a role.
Healing after implant surgery depends on the body’s ability to recover normally. If you have a medical condition that affects healing, your dental and medical history may need a closer review. The key issue usually isn’t the diagnosis itself. It’s whether the condition is well managed.
That’s why candidacy conversations are individualized. Two people with the same medical label may not have the same treatment plan.
Good implant planning is less about checking boxes and more about understanding how your mouth and your body heal.
Lifestyle matters too
Daily habits can influence implant success.
Smoking, inconsistent brushing and flossing, and skipping follow-up care can all make healing less predictable. On the other hand, patients who are willing to care for their gums, keep regular appointments, and follow instructions usually give themselves a much better foundation for long-term success.
A good candidate often looks like this:
- Committed to oral hygiene because implants still need daily care.
- Willing to attend follow-up visits so healing can be monitored.
- Open to preparatory care if the bone or gums need attention first.
Candidacy can change over time
This is the part many people don’t realize. Implant candidacy isn’t fixed forever.
A patient who isn’t ready today may become a strong candidate after treatment that improves the health of the gums or rebuilds bone in the area. If you’ve already been told you have bone loss, it helps to learn more about bone grafting for dental implants because that step often changes the conversation from “not yet” to “possibly yes.”
That’s why a proper exam matters so much. The question isn’t only whether you qualify this minute. The question is whether there’s a safe path to get you there.
Your Path to Becoming a Great Implant Candidate
Hearing that you need a preparatory step can feel discouraging at first.
In reality, it’s often good news. It means there’s a strategy. Instead of forcing an implant into conditions that aren’t ready, the dentist improves the foundation first and gives the treatment a better chance to succeed.
Bone loss doesn’t always end the conversation
Bone loss is one of the most common reasons patients think implants aren’t possible. That’s understandable, especially if the tooth has been missing for a long time.
But lack of bone often leads to a treatment plan, not a dead end. Bone grafting can rebuild support in an area that has thinned over time. The purpose is straightforward. It creates enough healthy structure for an implant to sit more securely later.
In the verified data, bone grafting and related procedures are described as restoring volume in a high percentage of cases, and those interventions can help many patients move toward implant success when bone loss would otherwise be a barrier. The same data also notes that when bone support is inadequate and left unaddressed, failure risk can be much higher.
Gum therapy can change the outlook
Some patients have enough bone but not healthy enough gums.
That’s also treatable in many situations. Periodontal therapy reduces inflammation, controls infection, and gives the tissue a healthier environment before implant placement. If the gums bleed easily or there’s active disease, slowing down and treating that first is often the smartest move.
This can be hard for patients to hear because they want the replacement tooth right away. But healthy tissue is what makes the final result more predictable.
Sinus lifts and site preparation
Upper back teeth create a different challenge.
In that part of the mouth, the sinus area may leave limited room for an implant. A sinus lift creates more usable space by preparing the area and increasing the available support. It’s another example of how candidacy can be built in stages.
A site may also need smaller adjustments after extraction or after years without a tooth. The details vary, but the theme stays the same. Good implant care is foundation-first care.
Why preparation is a strength, not a setback
Patients sometimes think preparatory treatment means something has gone wrong.
It usually means the planning is careful.
- More accurate timing helps the dentist place the implant when the site is ready.
- Better support improves the chance of stable healing.
- Safer treatment reduces avoidable risks from rushing.
This is especially important for full-mouth reconstruction cases or for patients replacing teeth in visible areas where both function and appearance matter.
The best implant result often starts before the implant is ever placed.
If you’re trying to understand the sequence, this overview of a dental implant timeline can help you see how consultation, healing, placement, and final restoration fit together.
A “not yet” can become a “yes”
That shift is one of the most reassuring parts of implant dentistry.
Someone may come in with bone loss, inflamed gums, or an older dental problem they’ve been avoiding. After evaluation and preparation, that same person may become a solid candidate for treatment. The timeline may be longer than they hoped, but the goal is a result that’s built to last.
Vienna Implant and Family Dentistry provides implant care, bone grafting, full-mouth reconstruction, and related restorative treatment under one roof, which can simplify planning for patients who need both preparatory and final phases of care.
For many adults, the question isn’t “Am I perfect for implants right now?” It’s “Can a healthy path be built for me?” In many cases, the answer is yes.
Are Dental Implants Always the Best Choice?
A patient in Vienna might come in expecting implants and leave feeling surprised that the answer is, "Maybe, but let’s look at the full picture first."
That is a good thing.
Good implant planning is not about steering every person toward the same treatment. It is about matching the replacement to the mouth, the health history, the timeline, and the budget. For some patients, an implant is the closest match to a natural tooth. For others, a bridge or denture may be the smarter choice now, especially if they want to avoid surgery or need to replace teeth sooner.
Comparing Tooth Replacement Options
| Feature | Dental Implants | Fixed Bridges | Removable Dentures |
|---|---|---|---|
| Support | Placed in the jaw to support a replacement tooth | Supported by neighboring teeth | Rests on the gums |
| Effect on nearby teeth | Usually doesn’t rely on adjacent teeth for support | Typically requires reshaping nearby teeth | Doesn’t usually require reshaping nearby teeth |
| Feel in daily use | Often feels more like a natural tooth | Feels fixed in place | Can shift or feel bulky for some patients |
| Bone support | Designed to replace the root area as well as the visible tooth | Replaces the missing tooth space from above | Replaces missing teeth above the gums |
| Maintenance | Requires daily brushing, flossing, and follow-up care | Requires careful cleaning around the bridge | Must be cleaned and removed as directed |
| Best fit for | Patients seeking a stable, long-term replacement | Patients who want a fixed option without surgery | Patients who need a removable or simpler option |
Why implants often stand out over time
An implant works more like a rebuilt tooth than a surface replacement. The post sits in the jawbone, and the crown attaches above it. A bridge and a denture restore the visible part of the smile, but they do not replace the root under the gumline.
That difference matters in daily life. Many patients like implants because they feel stable when chewing and speaking, and they do not depend on neighboring teeth for support. Research reviews published by the National Institutes of Health on dental implant survival and success also describe implants as a predictable long-term treatment in appropriately selected patients.
Still, "predictable" does not mean "automatic."
A patient can be a strong implant candidate and still choose another option. Someone may prefer a bridge to avoid surgery. Another person may choose a denture as a temporary step while planning future care. Cost can also shape the decision, which is why it helps to review the full cost of dental implants and related treatment factors before deciding.
When another option may be the better fit
A bridge or denture may be reasonable if:
- You want a non-surgical solution and prefer to avoid implant placement.
- You need to replace a tooth quickly and implants are not the right timing yet.
- You are in a preparatory phase and your gums or bone need treatment before implant care.
- Your current budget fits another option better and you want a practical plan that works now.
That last point deserves honesty. Dentistry has to fit real life. A treatment plan is only helpful if a patient can move forward with it.
The right answer depends on where you are now, and where you want to go
Implants are often the strongest long-term option for replacing missing teeth, but they are not the only good option. The better question is whether they are the best fit for your situation today, or the best destination after some preparation.
For many patients, that is the part that brings relief. A bridge or denture does not always mean "never." It can mean "for now." And if bone grafting, gum treatment, or healing is needed first, the path to implants may still be open later.
The goal is not to force one answer. The goal is to choose the treatment that makes sense for your health, your comfort, and your next step.
Your Dental Implant Journey at Our Vienna Practice
Once a patient decides to explore implants, anxiety often shifts from “Am I a candidate?” to “What happens next?”
Most implant treatment is more manageable than people expect because it happens in stages. Each step has a purpose, and knowing that sequence tends to make the process feel much less overwhelming.
Step one is a detailed consultation
The first visit is where the plan becomes personal.
Your dentist reviews your dental history, medical history, bite, gum health, and the area of tooth loss. Imaging helps show bone shape, available space, and any conditions that need attention before treatment moves forward.
This is also when patients ask the questions they’ve been carrying around for months. Will this hurt? How long will it take? Do I need grafting? Can the tooth be replaced right away?
Some patients need a preparatory phase
If the bone or gums need attention, that treatment comes first.
This may include bone grafting, periodontal treatment, extraction site preservation, or other steps that improve the implant site. The waiting involved can feel frustrating, but it’s there for a reason. Stronger tissue leads to better stability.
Patients who want a practical overview of fees and planning often find it helpful to review how much dental implants cost before or after the consultation so the financial side is easier to understand.
Implant placement is a focused procedure
When the site is ready, the implant post is placed into the jaw.
This part is typically more controlled and precise than many patients expect. Local anesthesia is used, and some patients choose sedation options when anxiety is a major concern. After placement, the area begins healing and the bone starts bonding to the implant.
That healing period is an active part of treatment, not a pause. The body is doing the work that makes the implant stable.
The final tooth comes after healing
Once the implant has integrated well, the connector and final restoration are attached.
At that point, the missing space is no longer just covered. It’s restored with a replacement designed to function as part of your smile. For a single missing tooth, that usually means a custom crown. For multiple missing teeth, the design can be larger and more extensive.
Patients are often surprised that the process feels more organized than dramatic. Each stage has a clear job.
Age alone doesn’t rule you out
A lot of older adults assume implants are mainly for younger patients. That isn’t how candidacy works.
Verified data shows that about 9% of all dental implants in the U.S. are placed for patients ages 65 to 74, and 23% of people over 60 have no teeth, highlighting a significant need among seniors. The same source notes that age itself is not the barrier. Overall health is the key factor. Those figures come from reported dental implant statistics on seniors and implant demand.
For adults in Vienna and surrounding Northern Virginia communities, that matters. If you’re older and have been told, or have assumed, that implants aren’t for you, a proper evaluation may tell a different story.
Frequently Asked Questions About Dental Implants
Does getting a dental implant hurt
Most patients say the idea is scarier than the procedure itself.
During implant placement, the area is numbed so you shouldn’t feel sharp pain during treatment. Afterward, some soreness is normal, especially in the first part of recovery, but it’s usually described more like post-procedure tenderness than severe pain. If you’re anxious about dental treatment, ask about comfort options before the appointment so you know what support is available.
How do I know if I’m a good candidate
You can’t determine that from symptoms alone.
Some people with healthy-looking mouths still need imaging because the key question is what’s happening under the gums. Others assume they’ve lost too much bone and then learn there’s a workable treatment path. The only reliable way to answer who is a good candidate for dental implants is with an exam, imaging, and a review of gum health, bone support, medical history, and daily habits.
If I’ve been missing a tooth for years, is it too late
Not necessarily.
Longer tooth loss can increase the chance of bone shrinkage, but that doesn’t automatically remove implants as an option. Many patients need site preparation before placement. The timeline may be different, but delayed treatment does not always mean impossible treatment.
Can seniors get dental implants
Yes, many can.
Age by itself usually isn’t the deciding factor. Healing ability, gum health, bone support, and overall health matter more. Older adults often pursue implants because they want a more secure alternative to missing teeth or a removable prosthetic that no longer feels stable.
How long does the whole process take
It depends on your starting point.
A straightforward case moves differently from a case that needs extractions, bone grafting, or gum therapy first. Healing is part of the timetable, and that’s a good thing. Rushing implant treatment usually isn’t the goal. Building a stable result is.
Can I get an implant the same day a tooth is removed
Sometimes, but not always.
Same-day placement depends on the condition of the bone, the presence or absence of infection, the position of the tooth, and whether the site can support an implant immediately. In other cases, waiting is safer and more predictable. This decision should be based on the condition of your mouth, not on a one-size-fits-all promise.
Are implants hard to care for
They require commitment, but not complicated routines.
You still need brushing, flossing, and professional cleanings. Implants don’t get cavities, but the surrounding gums and bone still need protection. Patients who treat implants like natural teeth and keep regular follow-up care usually do better than patients who assume the implant is maintenance-free.
What if I’m embarrassed to come in because my mouth has gotten worse
You’re not alone, and you shouldn’t let that stop you.
Many adults delay care because life gets busy, money gets tight, or dental anxiety builds. Dentists see this every day. The useful question isn’t why you waited. It’s what your mouth needs now.
If you’re in Vienna, VA or nearby Northern Virginia and want a clear answer about whether implants are possible for you, schedule a consultation with Dr. Vikram Chauhan at Vienna Implant and Family Dentistry. A personalized exam can show whether you’re ready now or what steps can help you become a strong candidate for a lasting, confident smile.