You notice a little pink in the sink after brushing. It doesn’t hurt much, so it’s easy to shrug off and move on with your day.
That’s how gum disease often starts. Subtly. A small sign. No major pain. No emergency feeling.
The problem is that gums usually don’t bleed without a reason. If you’ve been wondering what happens if gum disease goes untreated, the short answer is this. It can move from mild irritation to infection that affects the tissue and bone holding your teeth in place, and it can also affect your options for future restorative care.
For adults in Vienna, VA and nearby Northern Virginia communities, this matters more than many people realize. Nearly 42% of U.S. adults age 30 and older have some form of periodontitis, and almost 60% of adults age 65 and older are affected, according to the CDC’s gum disease fast facts.
The good news is that gum disease is treatable, especially when it’s caught early. You’re not behind, and you don’t need to feel embarrassed. You just need clear information and a practical next step.
Your Guide to Gum Health in Vienna VA
A lot of patients assume bleeding gums come from brushing too hard. Sometimes technique plays a role, but frequent bleeding, puffiness, or tenderness usually points to inflammation.
That inflammation often begins with gingivitis, the earliest stage of gum disease. At this point, many people still feel fine. They can eat normally, smile normally, and carry on without realizing anything more serious is developing underneath the gumline.
Why small symptoms matter
Gum disease doesn’t usually begin with dramatic pain. It often starts with signs like:
- Bleeding when brushing or flossing
- Gums that look red instead of pink
- Persistent bad taste in the mouth
- Mild swelling along the gumline
- Tenderness when cleaning around certain teeth
Because those signs seem minor, people wait. They tell themselves they’ll floss more next week or schedule a cleaning when life slows down.
That delay is where trouble begins. Mild gum inflammation can often be managed before deeper damage happens. If it’s ignored, the infection can move below the gumline and affect the structures that support your teeth.
Simple rule: If your gums bleed more than once in a while, it’s worth getting them checked.
Why this is so common
Many adults are dealing with early gum problems without knowing it. Plaque builds up every day. If it isn’t removed well at home and during routine dental visits, the gums respond with irritation and swelling.
If you’re unsure whether what you’re seeing is normal, this page on signs of gum disease gives a helpful overview of the warning signs people often miss.
What patients usually want to know first
Patients aren’t asking for a technical lecture. They want answers to practical questions:
- Can this go away on its own
- Will I lose teeth
- Is bad breath related to my gums
- Could this affect implants later
- What can be done if I’m nervous about treatment
Those are the right questions. Gum disease isn’t just about your gums looking inflamed. It’s about whether the support for your teeth stays healthy over time.
From Reversible Gingivitis to Damaging Periodontitis
The easiest way to understand gum disease is to think of it in two stages. The first is irritation. The second is structural damage.
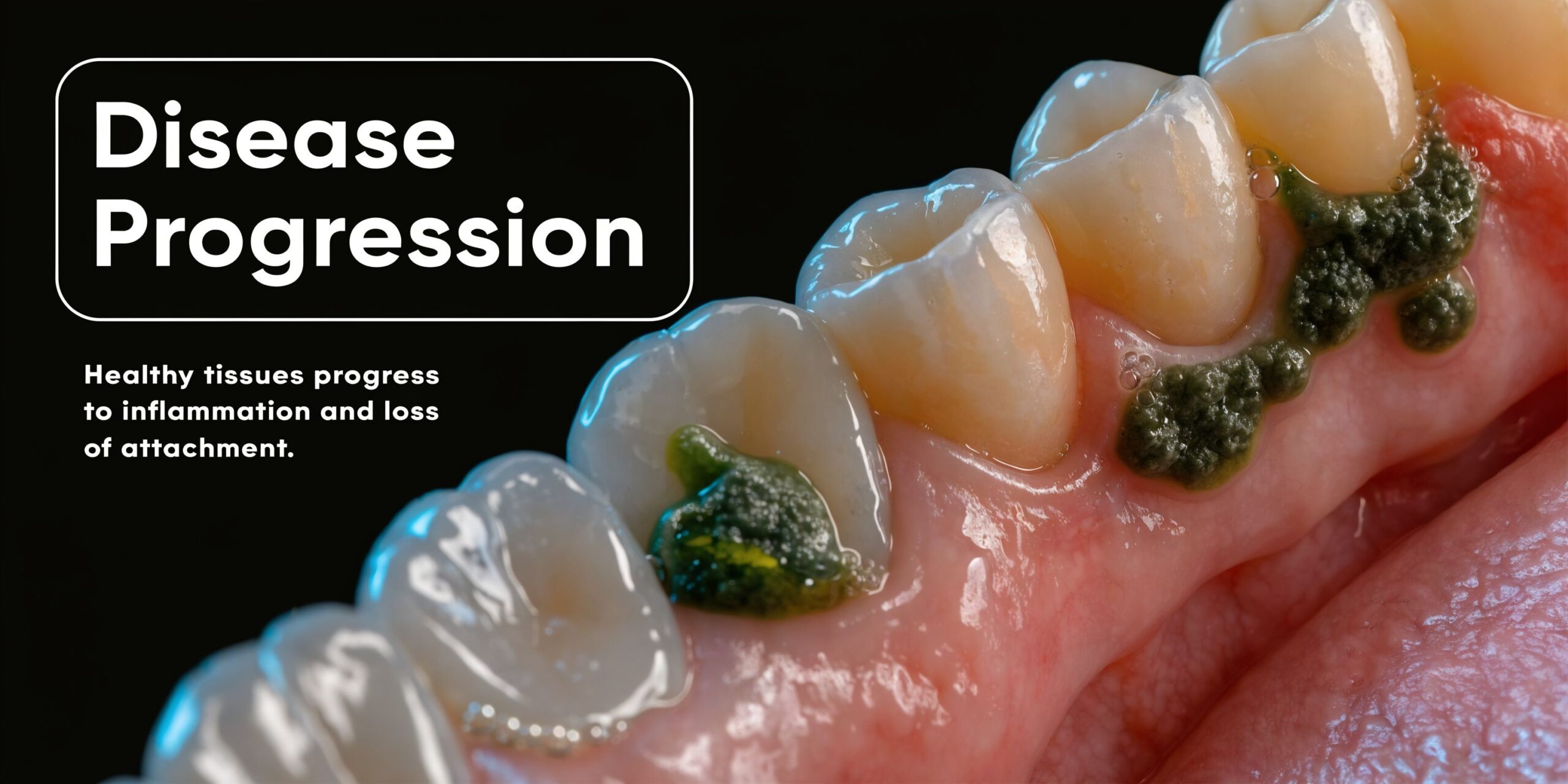
What gingivitis is
Gingivitis is the early stage. Plaque sits along the gumline, and the gums react by becoming swollen, red, and more likely to bleed.
At this stage, the damage is limited to inflammation in the gum tissue. That’s why gingivitis is considered reversible. If the bacterial buildup is removed and home care improves, the gums can often return to health.
A useful way to think about it is skin irritation. If your skin gets inflamed and you remove what’s causing it, the tissue can calm down. Gums work in a similar way early on.
What changes when periodontitis begins
Periodontitis starts when the problem goes deeper. The infection doesn’t just irritate the surface tissue anymore. It starts affecting the ligaments and bone that support the teeth.
According to this explanation of the danger of untreated gum disease, untreated gum disease can progress to periodontitis, where bacterial toxins destroy periodontal ligaments and alveolar bone, forming periodontal pockets deeper than 4 mm that harbor anaerobic pathogens like Porphyromonas gingivalis, leading to attachment loss and a significant risk of tooth loss within 5 to 10 years without intervention.
That sentence is clinical, so let’s put it in plain English.
When gums pull away from teeth, they create pockets. Those pockets trap bacteria in places your toothbrush and floss can’t clean well. Once that happens, the infection becomes harder to control with home care alone.
Why pockets are such a problem
A healthy gumline fits around the tooth fairly snugly. When infection causes separation, the space deepens.
That matters because:
- Bacteria stay protected below the gumline
- Inflammation becomes ongoing instead of occasional
- Bone support starts to break down
- Teeth lose stability over time
You may not feel this happening right away. That’s one reason periodontitis can advance further than people expect before they seek help.
Gingivitis vs. Periodontitis At a Glance
| Characteristic | Gingivitis (Early Stage) | Periodontitis (Advanced Stage) |
|---|---|---|
| Main issue | Gum inflammation | Infection affecting gums, ligaments, and bone |
| Common signs | Redness, swelling, bleeding | Recession, pockets, loose teeth, chewing discomfort |
| Reversible | Often yes, with timely care | No, the damage is considered irreversible |
| Where the problem sits | Mostly at the gum surface | Below the gumline in deeper supporting structures |
| Home care alone enough | Sometimes in very early cases | Usually no, professional periodontal treatment is needed |
| Long-term concern | Progression if ignored | Tooth instability and tooth loss risk |
Healthy gums don’t just look better. They act as the seal and support system around every tooth.
Where people get confused
Many people assume they’d know if they had advanced gum disease because it would hurt badly. That isn’t always true.
Some patients have serious inflammation, gum recession, or bone loss with very little pain. That’s why bleeding, bad breath, or a change in how the gums fit around the teeth shouldn’t be brushed off as minor.
How Untreated Gum Disease Destroys Your Smile
People often think gum disease is mostly a hygiene issue. In reality, it changes how your smile looks, how your teeth function, and what treatment options stay available later.
The visible changes usually come first
A smile affected by untreated gum disease may not look dramatically different overnight. The changes often show up gradually.
Common examples include:
- Bad breath that keeps returning even after brushing
- Gums that shrink back, making teeth look longer
- Dark spaces between teeth that weren’t there before
- A puffy or uneven gumline
- Tooth sensitivity near exposed roots
These are easy to dismiss as cosmetic annoyances. They’re usually signs of deeper inflammation.
Function starts to change after appearance does
As the support around teeth weakens, everyday tasks can become uncomfortable. Chewing on one side may feel easier than the other. Crunchy foods may become irritating. Some people notice a tooth that feels slightly different when they bite down.
That “slightly different” feeling matters. Teeth depend on bone and connective tissue for stability. If the infection continues, that support weakens further and teeth can begin to shift or loosen.
A loose tooth is rarely the first sign of gum disease. It’s usually the result of a problem that has been active for a while.
Tooth loss is only part of the story
When people hear “untreated gum disease,” they usually think of losing teeth. That can happen, but another issue often gets less attention. Bone loss in the jaw.
Bone loss changes the foundation of your mouth. Even if a damaged tooth is removed, replacing it isn’t always simple if the supporting bone has already receded.
Future treatment planning is particularly important in such cases. Patients who may one day need crowns, bridges, or implant treatment benefit from protecting the bone they still have now.
According to this explanation of what happens if early gum disease is left untreated, bone loss from advanced gum disease erodes the jaw density required for implant success, and untreated periodontitis patients have up to 3x higher implant failure rates compared with those who have healthy gums.
That doesn’t mean a history of gum disease automatically rules out implants. It means the disease needs to be controlled first, and in some cases rebuilding the foundation may be necessary before implant treatment can move forward.
When infection becomes urgent
Untreated gum problems can also flare into painful infections. Swelling, drainage, and sharp discomfort around one area may signal a more urgent issue than routine gum irritation.
If you’re dealing with sudden swelling or severe pain, it helps to know when a problem may need fast care. This page on whether a dental abscess is an emergency can help you understand those warning signs.
What preserving your smile really means
Saving a smile isn’t only about keeping teeth white or straight. It means preserving:
- Comfort when chewing
- Confidence when smiling
- Stable spacing between teeth
- Enough healthy bone for future restorative options
- The ability to keep natural teeth as long as possible
Once bone and attachment are lost, treatment becomes more involved. Earlier care is usually simpler, more conservative, and easier on the patient.
The Surprising Link Between Gum Health and Overall Wellness
Your gums don’t exist in isolation. They’re part of your body’s immune and circulatory systems, which is why a chronic infection in the mouth can affect much more than your smile.
How a gum infection affects the rest of the body
When gums are inflamed and infected, the tissue becomes easier for bacteria and inflammatory byproducts to pass through. That gives oral bacteria more opportunity to enter the bloodstream.
From there, the body responds with inflammation. That doesn’t mean every patient with gum disease will develop a major medical problem. It does mean the mouth can contribute to a broader burden on the body, especially in people who already have other health concerns.
The heart and blood vessel connection
One of the clearest concerns involves cardiovascular health. Untreated gum disease has been associated with higher risk for serious events involving the heart and blood vessels.
According to this discussion of the dangers of untreated gum disease, individuals with untreated gum disease can have two to three times the risk of heart attack or stroke.
For patients, the practical takeaway is straightforward. If your gums are chronically infected, that isn’t just a dental issue to put off until it becomes painful.
Why diabetes and gum disease often aggravate each other
Gum disease can be harder to manage when blood sugar is difficult to control. At the same time, ongoing gum inflammation can make diabetes management more challenging.
That creates a frustrating cycle for some adults. The gums stay inflamed more easily, healing can be slower, and the infection can become more stubborn over time.
If you have diabetes, bleeding gums shouldn’t be treated as a minor side issue. They deserve attention early.
Other body systems can be affected too
The mouth is one of the main entry points to the body. When harmful bacteria build up below the gums, that doesn’t stay neatly contained forever.
Clinically, untreated gum disease has also been linked to problems such as:
- Respiratory complications, including pneumonia when oral bacteria are inhaled
- Pregnancy concerns, including higher rates of premature birth and low birth weight
- Greater inflammatory burden in patients who already have other health conditions
Those links don’t mean gum disease acts alone. They do show why controlling oral infection is part of taking care of overall health.
The Alzheimer’s question families often ask
Many families in Vienna ask some version of this question. Can gum disease affect the brain?
The area of greatest interest involves Porphyromonas gingivalis, a bacterium strongly associated with periodontitis. Research has identified this bacterium in the brains of Alzheimer’s patients, suggesting it may play a role in neurodegeneration.
The same source above notes that P. gingivalis has been identified in the brains of Alzheimer’s patients, suggesting gum disease may be a modifiable risk factor for neurodegenerative disease.
That doesn’t mean gum disease directly “causes” Alzheimer’s in a simple, one-step way. Brain disease is more complicated than that. But it does support something important and practical. Gum health may be one of the risk factors families can address instead of ignoring.
For older adults, gum care is about more than keeping teeth. It may also be part of protecting independence, nutrition, and long-term quality of life.
Why this matters in daily life
Systemic links can sound abstract until you think about daily consequences. Sore gums can make people avoid brushing. Loose teeth can change what they eat. Bad breath can make them withdraw socially. Infection can become a source of stress they carry every day.
That’s why untreated gum disease deserves attention even when it still seems manageable. The mouth affects eating, speaking, confidence, and health in ways that add up.
Taking Control of Gum Disease with Periodontal Therapy
Hearing about the risks can feel heavy. Treatment, thankfully, is usually much more straightforward than people expect.
The first step is figuring out how advanced the disease is and where it’s active. Gum disease isn’t treated by guesswork. It’s treated by measuring, cleaning, and creating a maintenance plan that keeps the infection from returning.
What the exam usually involves
A periodontal evaluation is designed to answer a few specific questions:
- How inflamed are the gums
- Are there pockets around the teeth
- Has bone support changed
- Which areas need focused treatment
This often includes a visual exam, periodontal probing around the teeth, and imaging to evaluate the supporting bone. Patients are sometimes nervous about probing, but it’s a brief and routine way to understand what’s happening under the gumline.
What scaling and root planing actually means
The main nonsurgical treatment for gum disease is scaling and root planing. Many people know it as a deep cleaning.
The name sounds intimidating, but the goal is simple. Remove plaque, tartar, and bacteria from below the gumline, then smooth the root surfaces so the gums have a cleaner environment to heal against.
A standard cleaning focuses on areas above the gumline. A periodontal deep cleaning goes deeper because the infection is deeper.
What treatment may include
Depending on the condition of the gums, care may involve:
- Scaling to remove hardened buildup from the tooth surfaces and below the gums
- Root planing to smooth rough root surfaces where bacteria collect
- Targeted antibacterial support in areas where pockets are difficult to control
- Follow-up rechecks to see how the tissue responds after treatment
Some people improve with nonsurgical therapy and close monitoring. Others may need more advanced periodontal care if the disease has already caused significant breakdown.
Comfort matters during treatment
Dental anxiety is common, especially for patients who have been avoiding care because they already feel ashamed about their gums.
That anxiety deserves respect. Good periodontal care should feel calm, clear, and manageable. Numbing options are often used to keep treatment comfortable, and some patients benefit from additional relaxation support.
If you’ve heard the phrase deep cleaning and immediately felt tense, this page on laser deep cleaning of teeth may help you understand one comfort-focused approach patients often ask about.
Practical insight: The hardest part for many patients is booking the visit. The treatment itself is often easier than the weeks or months of worrying about it.
What you can do at home after professional care
Professional treatment addresses the bacteria you can’t fully remove on your own. Home care keeps the results going.
That usually means consistent brushing, daily cleaning between teeth, and keeping recall visits instead of waiting until something hurts. Patients who do well long term usually treat gum care as maintenance, not a one-time fix.
A calm way to think about treatment
You don’t need to assume the worst if your gums are bleeding. You also shouldn’t assume the problem will fade by itself.
A better approach is this. Find out what stage you’re in. Get the infection under control. Then protect the improvement with a maintenance plan that fits your mouth and your comfort level.
Life After Periodontal Treatment in Vienna VA
Once gum disease is under control, the focus changes. The job is no longer just stopping damage. It becomes preserving the result and rebuilding anything the disease has already affected.

Maintenance becomes the long-term strategy
Patients are sometimes surprised to learn that successful gum treatment is usually followed by ongoing periodontal maintenance. That’s because a mouth with a history of gum disease often needs closer monitoring than a mouth that has never had active periodontal infection.
These visits are designed to remove bacterial buildup before pockets deepen again and to spot small changes early.
Restorative care may come next
Some patients finish periodontal therapy and continue maintenance. Others need to repair the effects of past damage.
That may include treatment such as:
- Crowns for teeth that need added protection
- Bridges when one or more teeth are missing
- Dental implants after the gums are stable and the foundation is healthy enough
- Full-mouth reconstruction planning for more complex cases
The sequence matters. Restorative work lasts longer when infection is controlled first.
What this means for implant planning
Patients often ask if they can still get implants after gum disease. In many cases, yes, but the answer depends on the condition of the gums and bone at the time of planning.
The key idea is stability. The healthier and more stable the foundation, the better the odds for long-term success with implant treatment and other restorations.
Confidence often improves before the smile is fully rebuilt
One of the most meaningful changes after periodontal treatment is not purely cosmetic. It’s relief.
People often feel better because:
- Their mouth feels cleaner
- Bleeding decreases
- Chewing becomes less stressful
- They stop worrying that every symptom means they’re about to lose a tooth
That emotional relief matters. Dental problems can weigh on people for a long time before they finally address them.
Treatment doesn’t have to begin with a complete makeover. It often begins with making the mouth healthy enough to move forward safely.
Cost concerns are common and valid
Many adults delay treatment because they’re worried about affordability. That’s understandable.
What helps most is having a clear plan. When patients know which problems need attention first and which restorative steps can wait until later, care feels more manageable. Payment options and membership-style savings plans can also make ongoing maintenance easier to keep up with over time.
Schedule Your Consultation at Vienna Implant and Family Dentistry
Untreated gum disease can start with a little bleeding and end with much bigger problems involving your teeth, your jawbone, and your overall health. The encouraging part is that early action can change that path.
If you’ve been putting off care because you’re busy, nervous, or unsure whether the problem is serious enough, this is a good time to get clarity. You don’t need to diagnose it yourself. You just need a careful exam and a team that will explain your options plainly.
At Vienna Implant and Family Dentistry, patients receive personalized, judgment-free care in a relaxed setting. Whether you need a periodontal evaluation, restorative planning, help for a painful flare-up, or want to know if implants are still possible after gum disease, the team can guide you step by step.
Same-day emergency appointments are available for urgent issues, and online scheduling makes it easier to get started.
If you live in Vienna, VA or nearby Northern Virginia communities, schedule a consultation with Vienna Implant and Family Dentistry at 112 Pleasant St. NW, Suite H, Vienna, VA 22180. Taking care of your gums now can protect your smile, your comfort, and your future treatment options.