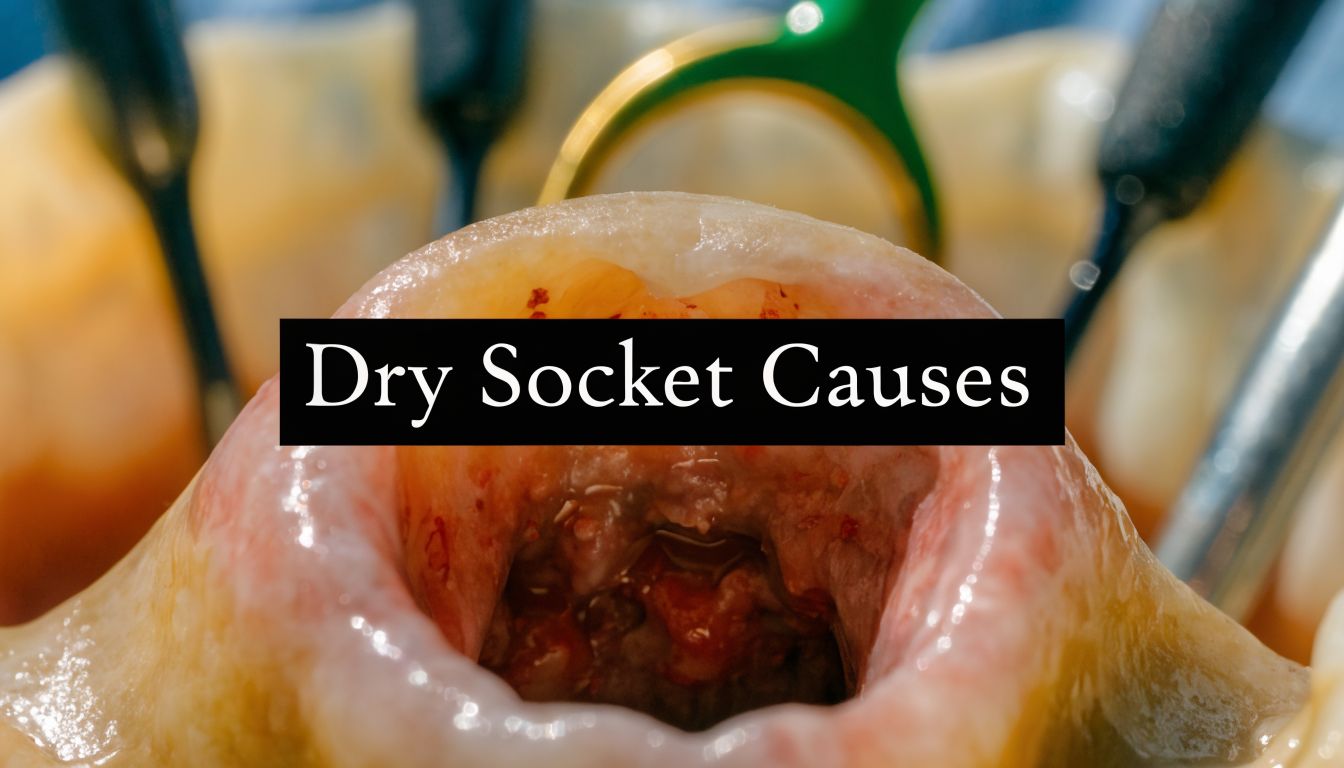
If you're reading this a few hours or a day after an extraction, you're probably doing what many patients do. You notice a twinge, feel the healing area with your tongue, and start wondering whether what you're feeling is normal or the start of a problem.
That worry is understandable. Dry socket sounds serious, and the name alone can make people uneasy. The good news is that it’s usually preventable, and if it does happen, it’s treatable. The key is understanding what causes dry socket after extraction, what raises your risk, and what signs mean it’s time to call.
Your Guide to a Smooth Recovery After a Tooth Extraction in Vienna VA
A common scene in any dental office goes like this. A patient gets home after an extraction, follows the instructions carefully, and still feels nervous once the numbness wears off. By the evening, they’re checking the site in the mirror and searching every symptom online.
That reaction makes sense. Your mouth has just gone through a procedure, and even normal healing can feel strange. Mild soreness, swelling, and tenderness often make people fear the worst before anything is wrong.
Why patients get confused after extractions
Part of the confusion is that the extraction site doesn’t look like a scraped knee or a cut on your hand. Healing in the mouth looks different. It can appear dark, uneven, or tender, and that alone can trigger concern.
Another reason is timing. Dry socket pain typically starts later than routine post-op discomfort, so some patients feel fine at first and then become alarmed when pain changes after a day or two.
Most people don't need to panic after an extraction. They need clear instructions, a calm plan, and someone to call if symptoms shift.
If you're also looking for practical advice on managing wisdom tooth extraction discomfort, that guide can help you think through the difference between expected soreness and symptoms that deserve attention.
The goal is healing, not guessing
A smooth recovery depends on protecting the extraction site in the first few days. That starts with understanding the blood clot, because that clot is the entire reason dry socket happens or doesn’t happen.
Once you know what the clot does, the rest of the advice makes more sense. No straw. No smoking. No forceful rinsing. No poking at the area. These aren’t random rules. They’re all about keeping that clot stable while your body does its job.
What Is a Dry Socket The Protective Blood Clot Explained
After a tooth is removed, your body immediately starts building a blood clot inside the empty socket. Think of it as your mouth’s version of a protective scab. It covers the space where the tooth used to be and shields the bone and nerves underneath.
That clot does two jobs at once. First, it protects the area from food, bacteria, and irritation. Second, it creates the foundation for normal healing.
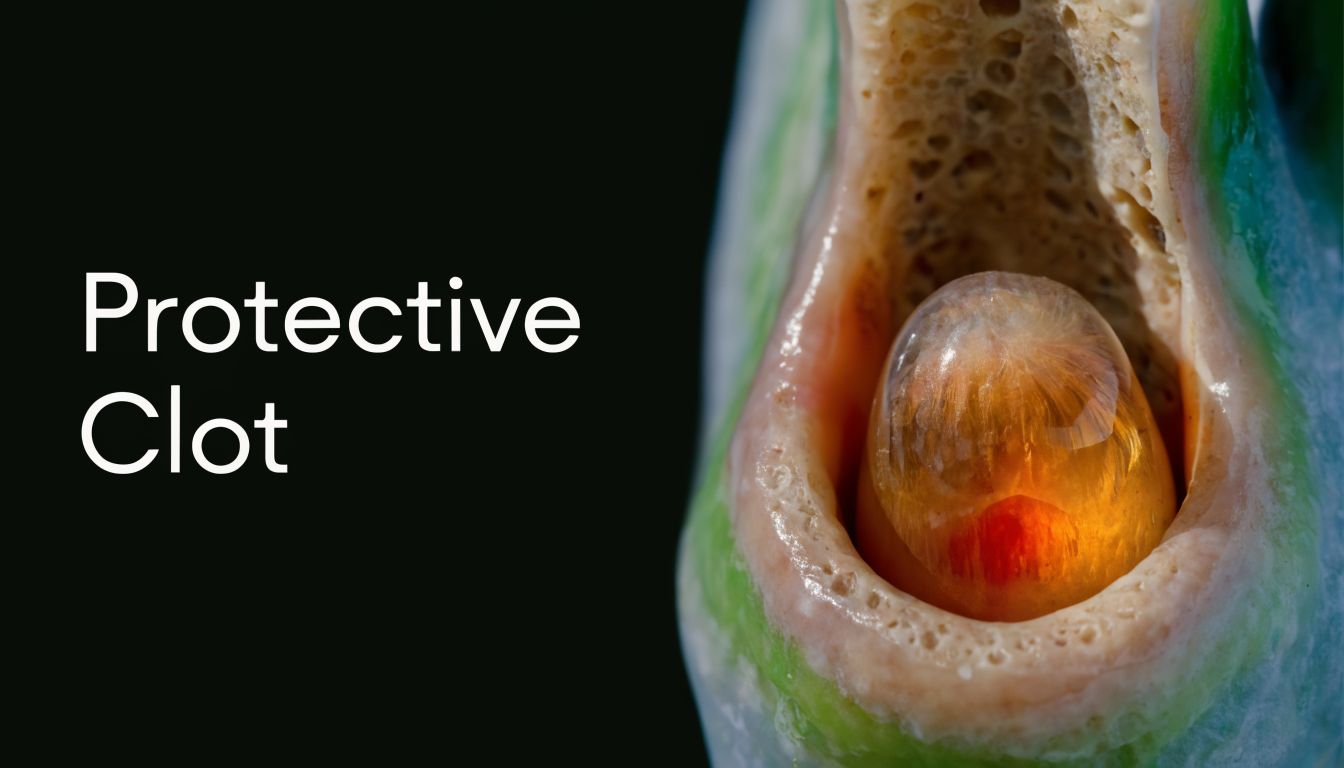
What dry socket actually is
Dry socket, also called alveolar osteitis, happens when that clot breaks down, dissolves too early, or gets dislodged. Once that barrier is gone, the socket is exposed. Bone and nerve endings no longer have the protection they need.
That’s why dry socket tends to hurt so much more than standard healing pain. According to this dry socket overview, dry socket arises primarily from the disintegration of the blood clot after extraction, often causing severe pain 1 to 3 days post-extraction. The same source notes that dry socket occurs in 1 to 5% of routine extractions, but can rise to 30% in third molar surgeries.
Why the pain feels different
Normal healing discomfort usually feels sore, achy, or tender. Dry socket pain is different because the socket loses its natural covering. Air, fluids, food debris, and bacteria can irritate exposed tissue much more directly.
People often get confused here because they assume a dry socket means an infection. It can involve contamination and irritation, but the central problem is loss of the clot.
A simple way to picture it
- Healthy healing means the clot stays in place and the site remains protected.
- Dry socket means the clot is missing or has broken down too soon.
- Pain increases because the tissues underneath are exposed instead of cushioned.
Practical rule: If the extraction site loses its protective clot early, healing becomes more painful and more vulnerable to irritation.
Why this matters for prevention
Once you understand the clot, aftercare instructions stop sounding overly cautious. Suction, smoking, rough rinsing, and certain foods all matter because they can disturb the healing site while that clot is still fragile.
This is the heart of what causes dry socket after extraction. It isn't bad luck alone. It's usually a disruption of the body’s early healing process.
Common Causes and High-Risk Factors to Understand
Some patients have one obvious risk factor. Others have several smaller ones that add up. Dry socket usually develops because the clot is either disturbed mechanically, broken down biologically, or both.

Surgical difficulty matters
One of the biggest causes is surgical trauma. A simple extraction usually heals more predictably than one that takes longer, involves more force, or requires bone removal or sectioning.
A review of third molar cases reported in this clinical article on alveolar osteitis found that dry socket in lower third molar extractions can reach 30 to 41.2%, compared with 1 to 5% in routine procedures. The same source notes that difficult extractions and poor oral hygiene both contribute to clot breakdown.
If you’re preparing for a procedure, it helps to review how to prepare for tooth extraction so you can reduce avoidable risks before treatment day.
Smoking, suction, and oral habits
Smoking is a major concern for two reasons. The chemicals in smoke can irritate the healing site, and nicotine reduces blood flow. That makes it harder for the socket to maintain a strong, stable clot.
Suction can cause problems too. Straws, forceful spitting, and aggressive rinsing create movement at exactly the wrong moment. Even if the clot has formed, it can still be fragile early on.
Site and anatomy also play a role
Lower back teeth, especially wisdom teeth, are more vulnerable. The anatomy of the lower jaw can make healing more challenging, particularly after a surgical extraction.
A few factors often combine:
- Procedure complexity increases tissue trauma.
- Poor oral hygiene raises the chance of contamination around the socket.
- Smoking after extraction makes clot stability harder to maintain.
- Lower wisdom tooth sites tend to be more prone to dry socket than simple upper extractions.
Some patients focus only on the straw rule. In real life, risk often comes from a combination of extraction difficulty, oral hygiene, and habits during recovery.
Biological influences you shouldn't ignore
Hormonal factors can matter as well. Estrogen can affect clot stability, which is why some women, especially those using oral contraceptives, may face higher risk. Age and personal healing patterns can also influence recovery.
That doesn't mean dry socket is inevitable if you have one of these factors. It means your dentist should know about them in advance so aftercare can be more personalized.
Your Personal Risk Profile Understanding Genetic Factors
Some patients ask a fair question. Why did I get dry socket before when I followed the instructions?
Sometimes the answer may involve your own biology. Not every person forms, stabilizes, and protects a clot in exactly the same way. That’s why a patient’s history matters so much.
Why past experience matters
According to this explanation of dry socket causes, people who’ve had dry socket before are at significantly higher risk of getting it again. That pattern suggests there may be a genetic component related to fibrinolytic activity or clot stability.
That doesn’t mean there’s a routine genetic test used in everyday dental visits. It does mean your dentist should take your history seriously.
What a personalized prevention plan can include
If a patient has had dry socket before, the conversation should be more detailed. Your dentist may want to review:
- Previous extraction experiences and how healing went
- Smoking or vaping habits before and after treatment
- Hormonal medications that could affect clot stability
- Sedation options if reducing stress and movement may help support a smoother procedure
Patient history helps guide prevention. It may influence pre-op rinses, the timing of treatment, and how closely the office follows your healing afterward.
If you've had dry socket once, say so before your extraction. That single detail can change the prevention plan.
Individualized care matters most. Two patients can have the same tooth removed and need different aftercare strategies based on their history.
Dry Socket Symptoms vs Normal Healing Pain
The hardest part of recovery for many people is not the soreness itself. It’s uncertainty. Patients often ask, “Is this still normal?”
A useful rule is this: normal healing usually trends better, while dry socket usually feels like a turn in the wrong direction. Instead of gradually easing, the pain becomes sharper, deeper, or more intense.
What normal healing tends to feel like
Normal post-extraction discomfort is usually centered around the site. The area may feel tender when you bite, sore when the numbing wears off, or mildly irritated with jaw movement. That can be unpleasant, but it should slowly settle.
Dry socket tends to announce itself differently. The pain often feels more severe, more persistent, and out of proportion to what patients expected. Some people also notice a bad taste, unpleasant odor, or a socket that looks unusually empty.
Is It Dry Socket? A Symptom Comparison
| Symptom | Normal Healing | Potential Dry Socket |
|---|---|---|
| Pain pattern | Soreness that gradually improves | Pain that worsens instead of easing |
| Timing | Most noticeable soon after extraction, then slowly settles | Often becomes more concerning after the first day or two |
| Socket appearance | Looks like it is filling in and healing | May look empty or lacking the usual dark protective clot |
| Taste or odor | Mild post-op taste can happen | Bad taste or odor is more concerning |
| Reaction to eating or drinking | Mild tenderness is common | Sharp irritation at the site can occur |
| Overall sense | Feels like a normal surgical recovery | Feels like healing has stalled or reversed |
When your instincts are right
Patients are often accurate when they say, “This doesn’t feel like normal healing.” If pain suddenly intensifies, starts radiating, or seems far worse than expected, it’s worth a call.
You do not need to diagnose yourself perfectly at home. You only need to notice that the pattern has changed and let your dentist evaluate it.
How to Prevent Dry Socket After Your Tooth Extraction
Prevention is mostly about protecting the clot while the site is fragile. That means avoiding anything that pulls on it, irritates it, or fills the socket with debris.

The first habits matter most
The basic rules are simple, but they work best when you understand the reason behind them.
- Skip straws and suction. Pulling through a straw can disturb the clot.
- Don't smoke during early healing. Smoke and nicotine make clot stability harder to maintain.
- Avoid forceful rinsing. Gentle care protects the site better than aggressive cleaning.
- Leave the area alone. Touching it with your tongue or fingers can irritate the socket.
For more practical recovery steps, review aftercare for extractions before your procedure or while you're healing.
Food choices can help or hurt
Diet gets oversimplified after extractions. “Eat soft foods” is good advice, but not complete advice. Food texture matters because tiny particles can get trapped in the socket.
According to this dry socket aftercare resource, small hard particles from foods like rice or nuts can lodge in the socket, encourage bacterial growth, and contribute to clot dissolution. The same source recommends smooth, nutrient-dense foods during the first few days.
Good early choices usually include:
- Smooth foods like yogurt, mashed potatoes, soups that aren’t too hot, and applesauce
- Protein-rich options that are easy to eat, such as eggs or blended foods
- Plenty of water without using a straw
Foods to be careful with:
- Rice and small grains that can pack into the socket
- Nuts, seeds, and crunchy snacks that can scrape or lodge in the area
- Sticky foods that cling around the extraction site
Healing is easier when food nourishes the body without collecting in the socket.
Gentle cleaning is still important
Patients sometimes think they should avoid the area completely. That’s not the goal. You want a clean mouth without disturbing the extraction site.
After the initial post-op window, gentle rinsing and careful brushing around the area are usually part of good healing. Follow the specific instructions your dentist gives you, because timing matters.
Treating Dry Socket at Vienna Implant and Family Dentistry
If dry socket happens, the right treatment can make a big difference quickly. Patients often fear they’ve done lasting damage, but in most cases the main issue is pain control and helping the site heal more comfortably.
Treatment is usually straightforward and focused on relieving symptoms while protecting the area from further irritation.
What treatment often involves
A dentist may gently clean the socket to remove trapped debris. If food particles or irritants are sitting in the site, removing them can reduce ongoing inflammation.
After that, a medicated dressing may be placed in the socket. This dressing helps soothe the exposed area and can make the patient much more comfortable.
Comfort matters during treatment
People with dental anxiety often worry that treatment for dry socket will hurt. In reality, the goal is the opposite. The visit is meant to reduce pain, not add to it.
In a comfort-focused office, the team can explain each step before doing it. For anxious patients, sedation options may also be discussed when appropriate so treatment feels manageable and calm.
If your dentist talks with you about prescription pain control, it helps to understand how medications are used and what precautions matter. This guide to acetaminophen and codeine offers general medication background that some patients find useful before discussing options with their doctor or dentist.
Dry socket is painful, but it is also manageable. The sooner it's treated, the sooner patients usually feel relief.
Why prompt care helps
Waiting usually doesn't make dry socket “settle down” on its own in a comfortable way. If the pain is escalating, getting the site examined can spare you unnecessary suffering.
A prompt visit also lets your dentist make sure the problem really is dry socket and not something else that needs a different approach.
When to Call Your Vienna Dentist for Emergency Care
There’s no prize for waiting out severe dental pain. If your recovery feels off, call. A short conversation with the office can tell you whether what you’re experiencing sounds routine or needs same-day attention.
Signs you shouldn't ignore
Reach out if you notice any of the following:
- Pain that becomes intense instead of improving
- A bad taste or odor that doesn't go away
- A socket that looks empty or unusual
- Pain medication that isn't giving enough relief
- Swelling, drainage, or other symptoms that feel concerning
Patients often talk themselves into waiting one more day. That’s understandable, but it can leave you uncomfortable longer than necessary.
When same-day care makes sense
If pain is severe, worsening, or keeping you from eating, sleeping, or functioning normally, ask about same-day tooth extraction and emergency dental care. Quick evaluation matters when symptoms are escalating.
You don't need to be certain that it's dry socket before calling. You just need to know that healing doesn't seem to be following the normal path.
Dry socket can sound frightening, but it becomes much less intimidating once you understand the cause. The central issue is loss of the protective blood clot. From there, risk factors, prevention, symptoms, and treatment all start to make sense.
If you’re in Vienna, VA or nearby Northern Virginia and you’re worried about post-extraction pain, Vienna Implant and Family Dentistry is here to help. Dr. Vikram Chauhan and the team provide clear aftercare guidance, personalized treatment planning, sedation options for anxious patients, and same-day emergency support when recovery doesn’t feel right. If you have questions about healing, dry socket symptoms, or an upcoming extraction, contact Vienna Implant and Family Dentistry to schedule an appointment.