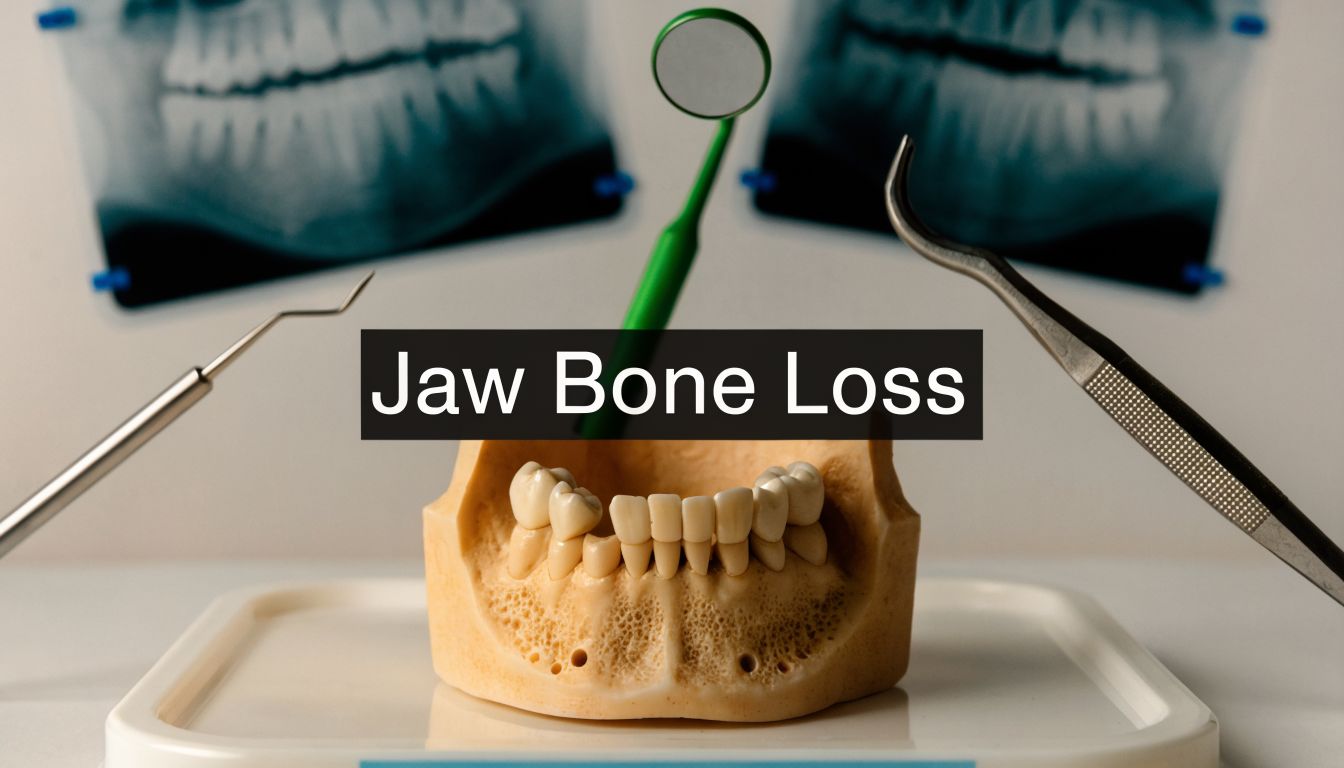
You notice something small at first.
A tooth feels a little different when you bite down. Your gums look lower in one area. A denture that used to fit fine starts to shift. Maybe you haven’t lost a tooth at all, but your smile looks a bit less full than it used to, and you can’t quite explain why.
That uncertainty makes people nervous. Many patients worry they’ve done something wrong, or that bone loss in the jaw means they’ve waited too long. In most cases, neither is true. Jaw bone loss is common, it often develops unnoticed, and it can happen for more than one reason.
If you’ve been searching for what causes bone loss in the jaw, the most helpful place to start is with a clear explanation of how the jaw works, what can damage it, and what can be done to protect or rebuild it. For families in Vienna, VA and nearby Northern Virginia communities, that understanding matters whether you’re thinking about preventive care, restorative dentistry, or dental implants near me.
Your Guide to Jaw Bone Health from a Dentist in Vienna VA
Many people think about teeth and gums as separate from bone. They’re not.
Your teeth sit in bone, and that bone needs steady support to stay strong. When infection, missing teeth, pressure changes, or whole-body health factors interrupt that support, the jaw can begin to shrink. Sometimes the change is slow enough that you don’t notice it until a tooth loosens or your facial shape changes. Other times, patients first learn about it when they ask about implants or a bridge.
That’s one reason this topic feels confusing. Patients often ask questions like:
- “Why are my teeth shifting?” Sometimes the supporting bone has changed.
- “Why does my lower face look different?” Bone loss can reduce support for the lips and cheeks.
- “Why is this happening if I brush and floss?” In some cases, the cause isn’t just hygiene.
- “Can this be fixed?” Often, yes. The right treatment depends on the cause and how much bone remains.
Jaw bone loss is serious, but it’s also manageable. Early diagnosis can make a major difference because treatment is often simpler before the problem advances.
A helpful mindset: Bone loss isn’t a personal failure. It’s a health condition with causes we can identify and address.
For local families, this issue also connects to everyday dental care. A child’s orthodontic development, an adult’s gum health, a parent’s loose denture, or a grandparent’s missing teeth can all involve the condition of the jawbone. That’s why family dentistry and restorative dentistry often overlap more than people expect.
If you’ve felt unsure about whether your symptoms matter, they do. A small change in fit, comfort, or appearance can be your first clue that the foundation under your smile needs attention.
The Foundation of Your Smile Understanding Jaw Bone Health
Your jawbone is the foundation of your smile.
A simple way to picture it is to think about a house. The roof and walls get most of the attention, but the whole structure depends on what sits underneath. Teeth are similar. They’re the visible part, but the bone around them is what keeps them stable and functional.
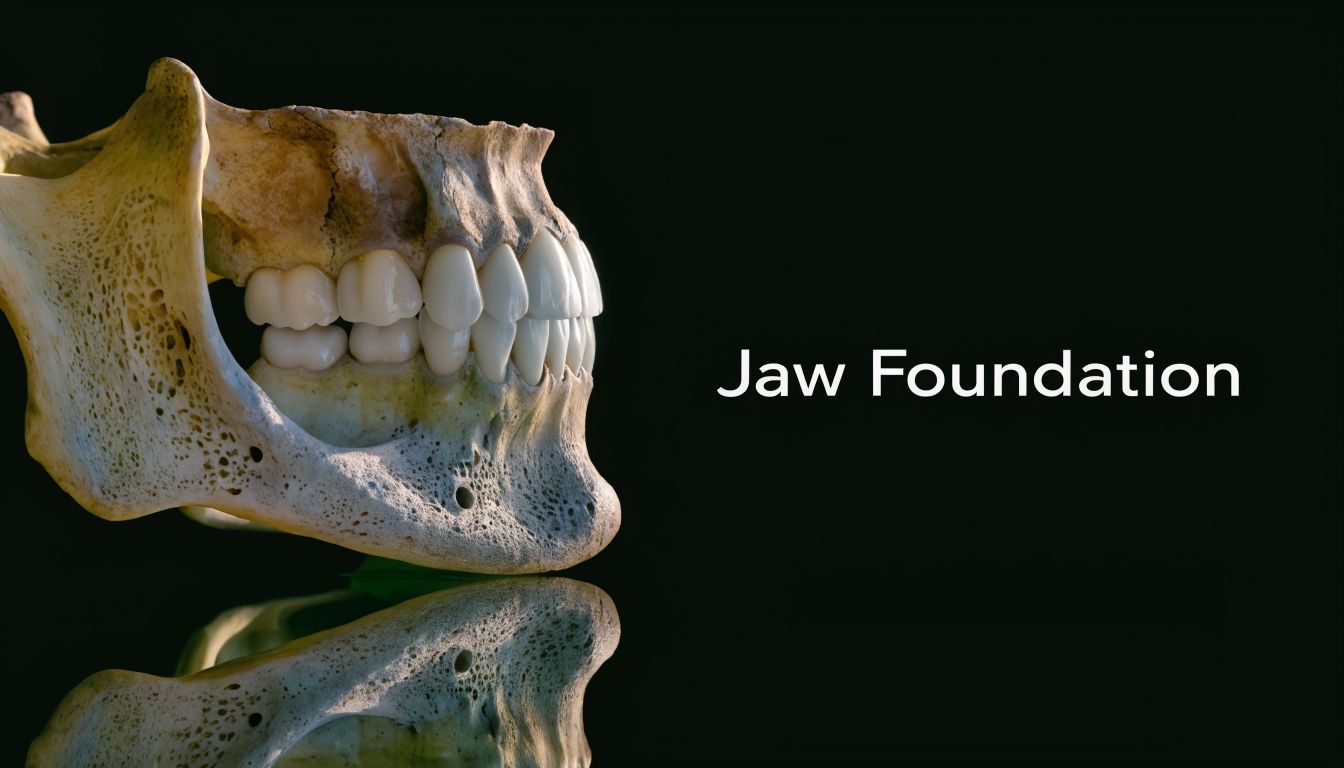
What the jawbone actually does
The part of the jaw that holds teeth is often called the alveolar bone. You don’t need to remember that term. What matters is what it does.
It helps:
- Anchor your teeth so they stay firm when you chew
- Support your bite so upper and lower teeth meet properly
- Maintain facial shape by giving structure to your lips and cheeks
- Create a stable base for restorations like implants
When the bone is healthy, it handles chewing forces every day. That pressure matters. Your body uses it as a signal that the bone is needed.
Why the body removes bone
Bone is living tissue. It’s always being renewed.
When a tooth root is present and functioning, chewing sends regular stimulation into the jaw. Your body reads that as “keep this bone.” If that stimulation drops, the body may begin to remove bone from that area because it no longer sees the same demand.
Patients often find this aspect confusing. They assume bone is permanent unless there’s an injury. In reality, the jaw responds to use, inflammation, and overall health.
Your body is efficient. If part of the jaw no longer supports a tooth or stays inflamed for too long, the body may reduce bone there.
Why bone loss changes more than your teeth
Bone loss doesn’t just affect whether a tooth feels loose.
It can also change:
- How your smile looks
- How dentures fit
- How easy it is to place implants
- How your face is supported over time
When enough bone is lost, lips and cheeks may look less supported. Some patients describe this as a more tired or sunken appearance. They notice it in photos before they notice it in their mouth.
That’s why jaw bone health matters even if you’re not in pain. The bone under your gums influences comfort, function, and appearance all at once.
The Primary Culprits Common Causes of Jaw Bone Deterioration
Some causes of jaw bone loss are much more common than others. The big ones are gum disease, missing teeth, severe infection, trauma, and bone changes in the upper back jaw after molars are removed.
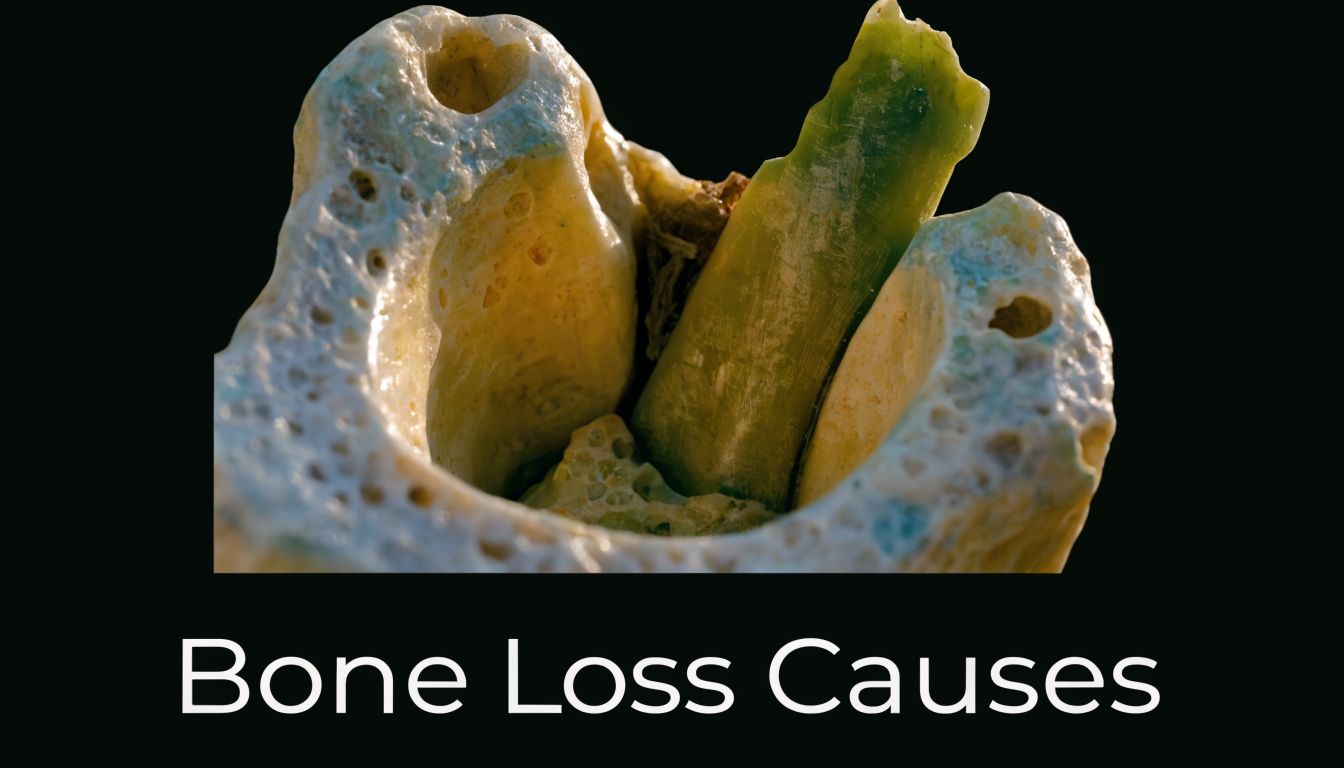
Gum disease
The most important cause to understand is periodontitis, which is advanced gum disease.
It isn’t just irritated gums. It’s a chronic infection below the gumline that triggers inflammation and gradually destroys the structures that hold teeth in place, including the supporting bone. Periodontitis is the leading cause of jawbone loss in adults worldwide, and it affects approximately 50% of adults over 30 globally while contributing to 70% of tooth loss in older populations, according to this review on the silent threat of bone loss.
Here’s what makes it dangerous. Plaque and bacteria build up under the gums. The body responds with inflammation. Over time, that inflammatory process damages attachment around the teeth and starts breaking down the bone.
Patients don’t always feel pain early on. That’s why gum disease gets missed.
Common clues include:
- Bleeding while brushing
- Gums that look puffy or receded
- Bad breath that keeps coming back
- Teeth that feel loose or shifted
- Spaces that seem new
If untreated, this process doesn’t stay confined to the gums. It moves deeper.
Missing teeth and the use-it-or-lose-it problem
When a tooth is removed or lost, the bone in that area loses its normal stimulation.
The root of a natural tooth helps transmit biting force into the jaw. Once that root is gone, the body may begin to resorb bone there. Patients often think replacing the visible tooth is the only issue, but the missing root is a big part of the story.
This is one reason traditional removable dentures can become less stable over time. They restore appearance and some function, but they don’t replace the root in the bone. Without that deeper stimulation, the jaw can continue to change.
A practical example helps. If you lose a back tooth and leave the space open, you may still chew on the other side and feel mostly fine. Meanwhile, the unused bone in the missing-tooth area can gradually shrink. Later, when you want an implant, there may be less bone available than you expected.
Severe tooth infections
A deep infection around the root of a tooth can also damage the surrounding bone.
When bacteria spread beyond the inside of the tooth and into nearby tissues, the body mounts an inflammatory response. That can destroy bone around the affected area, especially if treatment is delayed.
Patients sometimes assume that once the pain calms down, the problem has passed. It hasn’t. Some dental infections drain or quiet temporarily while the damage continues below the surface.
Signs that may point to this kind of problem include:
- Swelling near one tooth
- A bump on the gum
- Pain with biting
- A history of a broken or badly decayed tooth
Trauma and injury
A fall, sports injury, accident, or fracture can damage the bone that supports teeth.
Sometimes the damage is obvious right away. Other times, a tooth survives the injury but the surrounding support is weakened. Years later, that area may show changes in stability or shape.
Trauma-related bone loss can also happen after a difficult extraction, especially if the area heals with reduced volume. What matters isn’t just whether the tooth came out, but how the surrounding bone responds afterward.
Upper molars and sinus-related bone loss
The upper back jaw deserves special attention because it behaves differently from other parts of the mouth.
Above your upper molars sits the maxillary sinus, which is an air-filled space. After a molar is removed, that sinus can expand downward into the space where tooth roots used to be. As that happens, the available bone height in the upper jaw can decrease.
This is one reason patients are sometimes surprised when they hear they need a sinus lift before an implant in the upper back jaw. They assume, “The tooth was there before, so there must still be plenty of bone.” Not always.
Loss in the upper back jaw is often a two-part problem. Bone shrinks after the tooth is lost, and the sinus may also move into that space.
This area can still be treated very successfully, but it requires careful planning.
When causes overlap
Many patients don’t have just one cause.
Someone may have mild gum disease, then lose a molar, then chew less on that side because it feels awkward. Another patient may have excellent brushing habits but develop bone loss after an extraction in the upper jaw. A third may lose bone around a tooth that had a long-standing infection.
That overlap matters because treatment has to match the actual reason for the loss. The answer for active gum disease is different from the answer for a healed missing-tooth site or a sinus-related defect.
Beyond the Obvious Systemic and Lifestyle Risk Factors
Not all jaw bone loss starts in the mouth.
Sometimes a patient does many things right, keeps regular cleanings, brushes well, and still develops changes in the jaw. That doesn’t mean the symptoms are imagined. It means bone health is affected by the whole body, not just the teeth.

Smoking and diabetes
Some health and lifestyle factors make bone breakdown more likely or make healing less predictable.
Smoking is a major example. It affects blood flow and makes it harder for tissues to respond well to inflammation. Diabetes can also influence how the body handles infection and healing. When those factors are present, existing dental problems may progress more quickly or respond less predictably.
Patients often think of these as “general health” issues, separate from dentistry. They’re not. The tissues around the teeth and jaw are part of that same body-wide system.
Osteoporosis and lower bone reserve
Bone density elsewhere in the body can matter in the mouth too.
If someone already has reduced bone strength, the jaw may have less reserve when challenged by gum disease, missing teeth, or chronic inflammation. That doesn’t mean every person with lower bone density will lose jawbone, but it can affect the speed and severity of change.
This is especially important in adults who are exploring implants or full-mouth reconstruction. The quality of bone helps guide treatment timing and whether grafting may be helpful.
Genetics and why some healthy people still lose bone
This is the part many patients have never been told.
Recent genetic research has identified specific gene variants linked to significantly faster jaw resorption rates, independent of gum disease, affecting 15% to 20% of adults, according to this review of bone loss in the jaw.
That matters because it gives a real answer to a frustrating question: “Why is this happening to me if I take good care of my teeth?”
Sometimes the reason isn’t neglect. Sometimes the body is more prone to losing bone.
People with strong home care can still notice:
- Unexpected gum recession
- Bone changes near missing teeth
- Faster changes than family members or friends
- Bone loss that seems out of proportion to plaque buildup
Hormones and peri-menopausal changes
Hormonal shifts can add another layer.
The same source notes that estrogen decline during peri-menopause can increase the rate of bone loss by up to 25% annually in some patients. For women in this stage of life, jaw changes may appear even when oral hygiene is excellent and daily habits are healthy.
That can be emotionally difficult. Patients often feel confused because they’ve been diligent for years.
A better way to look at it is this: good home care still matters, but it doesn’t cancel every biologic risk. It lowers avoidable risk while your dentist evaluates the factors you can’t see on your own.
A clean mouth doesn’t always mean a low-risk mouth. Biology, hormones, and medical history can change the picture.
Medications and medical treatment
Some medications and medical therapies can also influence jaw health and healing.
If you’ve had radiation in the head or neck area, treatment planning may need to be more careful. Certain bone-related medications can also affect how dentists approach extractions, grafting, and implant planning.
That doesn’t mean treatment isn’t possible. It means your medical history matters just as much as your dental history.
Recognizing the Signs and Diagnosing Bone Loss in Vienna
Jaw bone loss often starts subtly, but there are signs patients can watch for.
Signs you may notice at home
Watch for changes like these:
- Loose teeth that weren’t loose before
- Receding gums that make teeth look longer
- A bite that feels off when you chew or close
- A denture or partial that no longer fits well
- Visible shifts in tooth position
- Changes in facial support, especially around the lips
- A history of gum bleeding or chronic inflammation
If any of these sound familiar, it’s worth having the area examined. Bone loss isn’t always visible in the mirror, but the clues around it often are.
If you’re also wondering whether gum symptoms could be part of the problem, this page on the signs of gum disease can help you spot common warning signs.
What a dentist looks for
Diagnosis starts with a clinical exam, but it doesn’t stop there.
Your dentist checks the gums, tooth mobility, bite relationship, and the way the tissues fit around each tooth or missing area. If gum disease is suspected, periodontal probing helps measure the depth of the spaces around the teeth and detect attachment loss.
Unless identified and treated, active periodontitis can continue to destroy support.
Why imaging matters
Bone can’t be judged accurately by appearance alone.
If untreated, periodontitis can cause the jaw bone to erode at 0.2 to 1.0 mm per year vertically, which is why tools like CBCT scans and regular periodontal probing are critical for early intervention, according to this discussion of bone loss in the teeth.
A CBCT scan is a 3D image. Instead of a flat picture, it shows height, width, and shape of the bone in much more detail. That’s useful when a patient is considering an implant, a graft, or treatment for advanced gum disease.
Clinical reality: Good treatment planning depends on knowing how much bone is present, where it has been lost, and whether the loss is active or stable.
Why early diagnosis changes your options
This is the part patients care about most.
When bone loss is found early, treatment is often more conservative. You may be able to control gum disease before tooth mobility worsens. A fresh extraction site may be managed to preserve bone for a future implant. A poorly fitting denture may be adjusted before more changes develop.
Waiting doesn’t make the diagnosis clearer. It usually narrows the available options.
Rebuilding Your Smile Modern Treatments for Jaw Bone Loss
Jaw bone loss doesn’t mean you’re out of options.
Treatment depends on the cause, location, and amount of bone involved. Some patients need to stop active disease first. Others need to rebuild lost bone. Others are ready to replace missing teeth in a way that helps protect the jaw from further shrinkage.
Stopping the cause first
If gum disease is active, treatment starts there.
The infection and inflammation need to be controlled before long-term restorative work can succeed. If a tooth has a deep infection, that problem has to be addressed. If an extraction is needed, the site should be managed with future bone support in mind.
This step may feel less exciting than implants or cosmetic changes, but it protects every treatment that comes after it.
Bone grafting and site development
When there isn’t enough healthy bone in an area, a bone graft may help rebuild the foundation.
That can be done after an extraction to preserve the site, or later when preparing for an implant. In the upper back jaw, a sinus lift may be needed if the sinus has expanded downward and reduced the available height for an implant.
If you want a plain-language overview, this page on what bone grafting for dental implants is explains why grafting is sometimes part of treatment.
For upper-jaw bone loss related to sinus expansion after a molar extraction, hydraulic sinus lifts combined with simultaneous implant placement have shown a 95% success rate in preserving bone, while reducing total treatment time by up to 50% compared with traditional two-stage grafting, according to this review of causes of jawbone loss.
Why implants matter so much
A dental implant doesn’t just fill a gap. It replaces the missing root.
That root replacement is what makes implants different from traditional dentures and bridges in the context of bone health. Because the implant sits in the jaw, it can provide the kind of stimulation the bone has been missing.
For many patients, that makes implants the most biologically complete way to replace a tooth.
Vienna Implant and Family Dentistry provides implant planning, bone grafting, full-mouth reconstruction, implant-supported dentures, same-day CEREC crowns, and sedation dentistry as part of complete restorative care.
Comparing Treatments for Jaw Bone Loss and Missing Teeth
| Treatment | Impact on Jaw Bone | Best For | Lifespan |
|---|---|---|---|
| Bone grafting | Rebuilds or preserves bone volume in areas that need more support | Patients preparing for implants or protecting an extraction site | Varies by healing response and long-term maintenance |
| Dental implant | Helps stimulate the jaw because it replaces the root structure | Single missing teeth or stable long-term replacement | Long-term with proper care |
| Implant-supported denture | Provides more jaw stimulation than a traditional removable denture | Patients missing many or all teeth who want more stability | Long-term with maintenance and component replacement as needed |
| Bridge | Restores the visible missing tooth space but does not replace the root in bone | Patients who aren’t candidates for implants or want a non-surgical option | Long-term with proper care |
| Traditional denture | Restores appearance and some function but does not stimulate the jaw like a root-based option | Full-arch tooth loss when implants are not chosen or not possible | Varies and often needs adjustment or replacement over time |
Matching treatment to the person
Two patients with “bone loss” may need very different care.
One patient may need periodontal treatment and monitoring. Another may need a graft before an implant. Another may be best served by implant-supported dentures because their current denture moves too much and no longer feels secure.
The right plan isn’t based on guesswork. It’s based on the cause of the bone loss, the health of the remaining teeth, medical factors, and your goals.
Your Partner in Health Preventing Bone Loss in Vienna VA
The best treatment for jaw bone loss is prevention whenever possible.
That starts with regular dental visits, consistent home care, and early attention to symptoms that seem minor. Bleeding gums, a loose tooth, a shifting bite, or a missing tooth that’s been ignored for years can all change the jaw over time. Catching those issues early usually gives you simpler options.
Prevention also means acting before a small problem becomes structural. Replacing a missing tooth, treating gum disease promptly, and monitoring changes with routine exams can help protect the bone that supports your smile.
If prevention is your goal, this page on why preventative dentistry is the key to a healthy smile is a useful next step.
Patients with dental anxiety often put off care because they’re worried about discomfort, judgment, or hearing bad news. That hesitation is understandable. It’s also one of the biggest reasons small issues grow. A calm, clear consultation can make the situation feel much more manageable.
What individuals need isn’t pressure. They need answers.
That includes:
- A careful exam to find the cause
- A personalized plan based on health, goals, and comfort level
- Straightforward options for prevention, restoration, or implants
- Support for anxiety, including sedation when appropriate
If you live in Vienna, VA or nearby Northern Virginia and you’re worried about loose teeth, gum recession, missing teeth, or changes in your facial profile, schedule a consultation with Dr. Vikram Chauhan. A focused evaluation can show what’s causing the problem, whether bone loss is present, and what you can do next to protect or rebuild your smile.
Jaw bone loss is serious, but it’s not hopeless. Once you know the cause, you can make a plan.